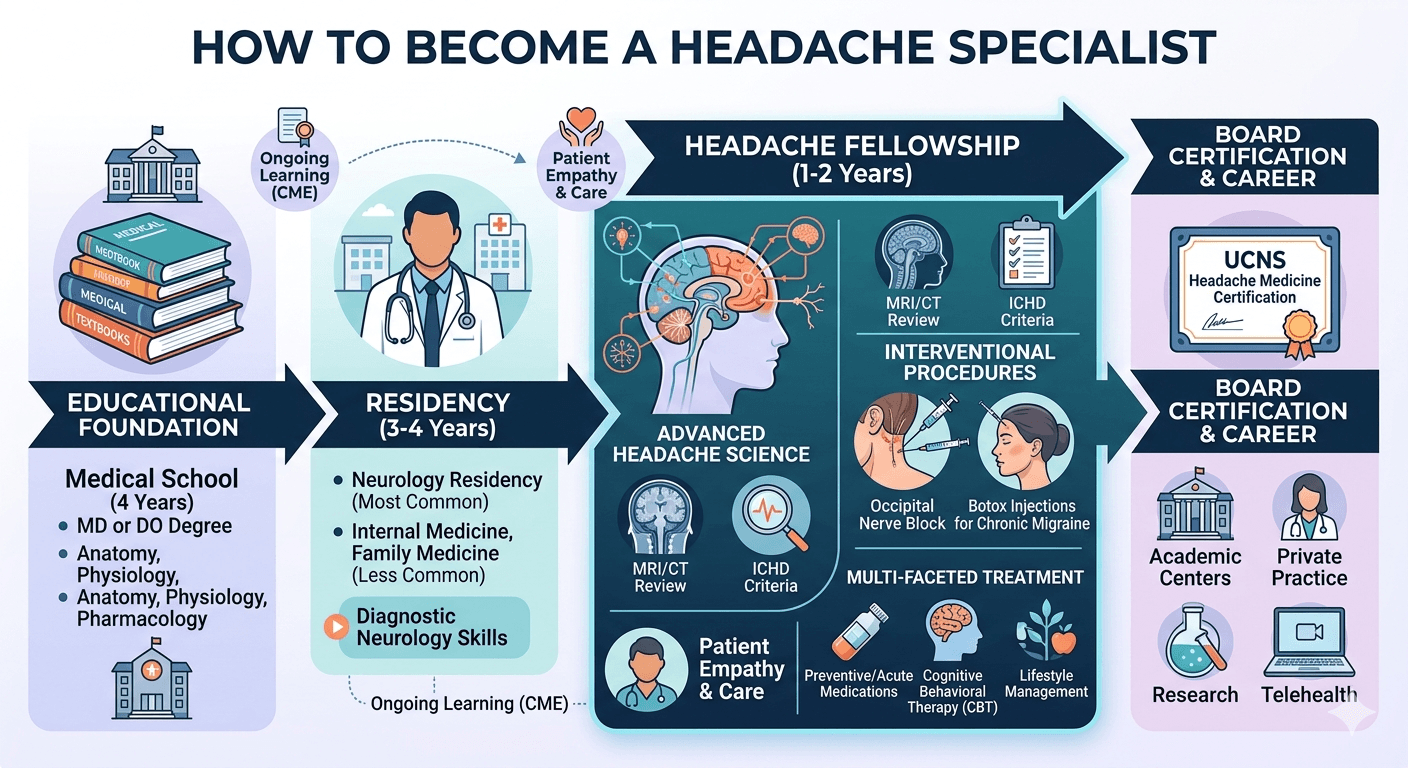
Why Seeing a Headache Specialist Is Different
Many patients are surprised to learn that not all neurologists are headache specialists. Migraine and other headache disorders are incredibly common, yet truly specialized care can still be hard to find. More than 40 million Americans live with migraine in the United States, but there are only around 700 headache specialists nationwide. That mismatch is part of why so many patients spend years searching for answers, cycling through treatments, or feeling like their symptoms are not being fully understood.
So what does it actually mean to be a headache specialist, and what kind of training does that involve?
The path starts with medical school, followed by neurology residency. During residency, neurologists are trained to diagnose and treat a wide range of conditions involving the brain and nervous system, including stroke, epilepsy, dementia, neuropathy, multiple sclerosis, and headache disorders. That foundation is essential, but for physicians who want to focus specifically on headache medicine, residency is usually not the end of training.
Headache medicine is a subspecialty within neurology. After residency, some neurologists go on to complete additional fellowship training focused specifically on headache disorders. That extra training is important because headache medicine is much more nuanced than most people realize. Migraine is not just a bad headache, and the field extends far beyond prescribing a few common medications.
A headache specialist is trained to diagnose and manage a wide range of headache disorders, including chronic migraine, cluster headache, new daily persistent headache, vestibular migraine, post traumatic headache, facial pain, and medication overuse headache. Just as importantly, a headache specialist learns how to sort through complicated presentations that do not always fit neatly into a simple category. Many patients have overlapping symptoms, multiple diagnoses, treatment side effects, sleep issues, hormonal influences, neck pain, anxiety, dizziness, or other factors that all need to be considered together.
That is one of the things I appreciate most about this field. It requires careful listening and thoughtful problem solving. Often the most important part of the visit is not just choosing a medication, but really understanding the pattern of symptoms, what has already been tried, what the patient is worried about, and how the headaches are affecting daily life. Good headache care is rarely one size fits all.
The training also includes learning how to use a broader set of treatments. Depending on the practice, this may include acute medications, preventive therapies, Botox, nerve blocks, infusion treatments, and other procedural options. It also means learning how to tailor treatment to the individual patient, taking into account side effects, other medical conditions, pregnancy planning, insurance barriers, and personal preferences.
For me, becoming a headache specialist meant years of training in neurology, followed by additional focused subspecialty training in headache medicine. It also meant choosing to center my career around this patient population because I saw how often patients with headache disorders were dismissed or minimized. Too many people are told their imaging is normal, that their symptoms are stress related, or that they simply need to live with it. In reality, headache disorders can be profoundly disabling, and they deserve the same level of seriousness and expertise as any other neurologic condition.
I think it is also helpful for patients to know that not every doctor who treats headache has completed advanced subspecialty training in headache medicine. That does not mean other physicians cannot help, because many absolutely can, but there is a difference between seeing headache as one part of a general practice and dedicated training. For patients with frequent, severe, unusual, or treatment resistant headaches, that difference can matter.
When patients ask why it can be so difficult to find a headache specialist, the answer is simple. There are not enough of us. When you compare more than 40 million Americans with migraine to only about 600 headache specialists in the country, it becomes much easier to understand why access is limited and why wait times are often long.
My goal is to provide thoughtful, evidence based, individualized care for people living with migraine and other headache disorders. Patients deserve to be taken seriously, and they deserve care from someone who understands how complex these conditions can be. That is what headache specialty training is really about.